TMJ/TMD Therapy With Our Holistic Dentists
Erase Jaw Soreness With Ease With TMJ/TMD Therapy
"TMD (Temporomandibular Joint Dysfunction) affects 5-12% of the entire population." (NIH 2014). Scott Udoff DMD PC's question to the NIH is what parameters were used to assess the TMD, because by the time a person experiences pain in the TMJ region, the dysfunction has existed for many years.
TMD is a chronic progressive disease leading to the complete derangement of the temporomandibular joint (TMJ). This derangement advances the unraveling of the homeostasis of the entire musculoskeletal system. The question is which dysfunction came first: TMD or musculoskeletal disharmony.
Studies have proven that the symptoms of TMD and musculoskeletal disharmony are a descending phenomenon. This means the symptoms of musculoskeletal dysfunction develop from TMD to cervical vertebrae and descend down the body. If you would like to learn more, please keep reading:
Temporomandibular Disorder (TMD)
To understand TMD, we first want to help patients understand the anatomy and function of the TMJ and joint space.
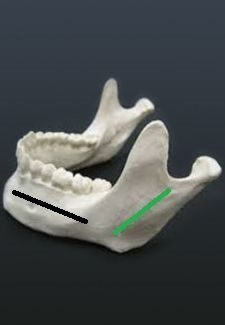
The lower jaw articulates in a space of the skull called the mandibular fossa (temporal bone of the skull). The lower jaw, called the mandible, has a vertical (green in the picture below) and horizontal (grey in the picture below) component. The horizontal component houses the teeth, and the vertical component is what articulates in the mandibular fossa. The end of the vertical component has an oval shape to it that’s longer left to right than up and down. This is called the condyle (marked with an arrow).
The condyle is covered with a thin layer of hard connective tissue. Housed between the condyle and mandibular (temporal) fossa is the articular disc. A fibrous tissue that resembles a donut, it allows the condyle 360 degrees of support due to the thinness in the middle with a thick, fibrous connective tissue ring.
The temporomandibular joint is encapsulated in a connective tissue sling that’s completely sealed so synovial fluid can lubricate the moving parts. The articular disc is attached from behind by inelastic connective tissue (retro-discal tissue) and in front by a muscle (the lateral pterygoid muscle).
As the jaw moves, the lateral pterygoid muscle must contract in order to keep the disc on top of the condyle. When the lateral pterygoid releases and the mandible closes, the inelastic connective tissue (that is attached from behind) is tight, allowing the disc to stay on top of the condyle as the jaw closes.
The masticatory system is composed of four compensating parts. All four on dependent on each other. They are:
- Teeth
- Periodontium (gums and bone)
- Temporomandibular joint
- Neuromuscular system
The teeth are the only part of the masticatory system that will not accommodate. For the system to work in physiologic harmony, the gears of the teeth must line up when the TMJ and neuromuscular system are in physiologic equilibrium.
The neuromuscular system is an intricate network of nerves and muscles controlled by neural feedback loops. There are 26 muscles attached to the mandible (lower jaw). They have a proprioceptive control mechanism where their action is controlled mainly by the arrangement of the gearing of the teeth. When the gearing of the teeth causes shifting of the mandible, the neuromuscular system responds rapidly by accommodating to the needs of the teeth, allowing them to “line up.” Any small, accommodating shifts will begin the process of joint derangement.
The signs and symptoms of TMD can be divided into three categories: muscle, non-muscle, and musculoskeletal.
Muscle pain is caused by a sustained accommodating muscle contraction, leading to constricted blood flow followed by depleted oxygen to the muscles.
Musculoskeletal Health
The head postures above the atlas and ondontoid process. The atlas and ondontoid process are the first two cervical vertebrae. The head rotates in all dimensions atop the atlas. Forty-two muscles are attached to the skull — short ones from the cervical vertebrae to the base of the skull and long ones from the sacrum up to the base of the skull.
This intricate system can contribute to the onset of TMD because of fatigue, injury, or general dysfunction. Thankfully, Dr. Udoff can serve as a personal guide for his patients, helping you understand the intricacies of your musculoskeletal health and how your symptoms relate to the presence of TMD. Effective therapy options will not be far behind once we’ve pinpointed the severity and cause of your condition.
Common muscle symptoms of TMD include:
- Temporal headaches (also called migraines)
- Occipital pain/headaches (base of the skull)
- Neck pain, either down the back neck or along the side of the neck
- Limited mobility of the neck up and down or side to side
- Retro orbital pain (pain behind the eyes)
- Lower back pain (just above the waistline)
- Jaw is tired/sore/stiff at waking
- Pain in the jaw when chewing, yawning, and occasionally when swallowing
- Pain at the corner of the lower jaw
- Pain in ear
- Pain on palpation of the TMJ
- Limited painless opening
Common non-muscle symptoms include:
- Popping or clicking of the TM joint
- Can’t find bite
- Deviation on opening
- Ringing in the ears
- Vertigo
- Clenching
- Toothache
- Abfractions (teeth chipping off at the gum region)
- Bone loss around roots of teeth
- Mouth breathing
- Dry mouth
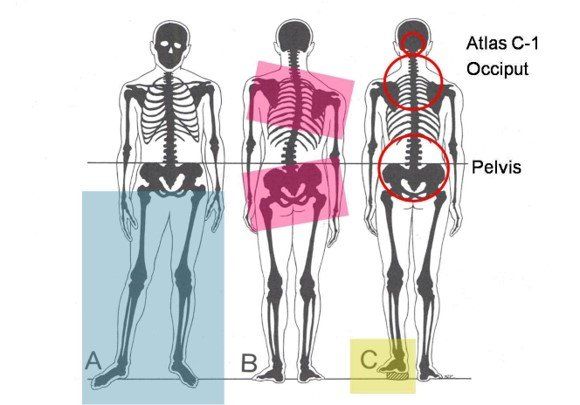
Common musculoskeletal symptoms include:
- Facial asymmetry
- Head pointed upwards
- Head postured forward
- Left and right shoulder sloping
- Pelvis imbalance (pelvic tilt)
- Protonation (inward roll of the foot)
- Changes in the curvature of the spine
What to Expect from Your TMJ Consultation
If you're dealing with pain in your mouth and jaw, you're not alone. In fact, over 10 million Americans suffer from TMJ disorder.
Call our holistic dentists near Rockland County, NY to book an appointment.
Here's what you can expect from your appointment with Dr. Udoff:
- Dr. Udoff will perform a gentle examination of your jaw and bite
- A 3D x-ray may be taken to help visualize what's going on in your mouth and jaw
- Dr. Udoff will help you understand what might be causing your TMJ pain
- Together, you'll develop a treatment plan to fit your needs and eliminate your TMJ pain for good.

Share On: